Uncontrolled urination, medically known as urinary incontinence, is a condition characterized by the involuntary leakage of urine. Far from just an embarrassing problem, it’s often a symptom of underlying issues affecting the urinary tract, impacting millions globally and significantly diminishing their quality of life. While it can occur at any age, it becomes more common with advancing age and can be linked to a variety of urinary tract diseases. Understanding the relationship between uncontrolled urination and these conditions is crucial for effective diagnosis and management.

Understanding Uncontrolled Urination (Urinary Incontinence)
Urinary incontinence isn’t a disease itself but a symptom. It occurs when the muscles and nerves that help hold or release urine don’t work properly. There are several types of uncontrolled urination, each with different underlying causes:
- Stress Incontinence: Leakage of urine when pressure is put on the bladder, such as during coughing, sneezing, laughing, exercising, or lifting heavy objects. It’s often due to weakened pelvic floor muscles and/or a weakened urethral sphincter.
- Urge Incontinence (Overactive Bladder): A sudden, intense urge to urinate immediately followed by involuntary urine leakage. This is often caused by an overactive bladder muscle that contracts involuntarily.
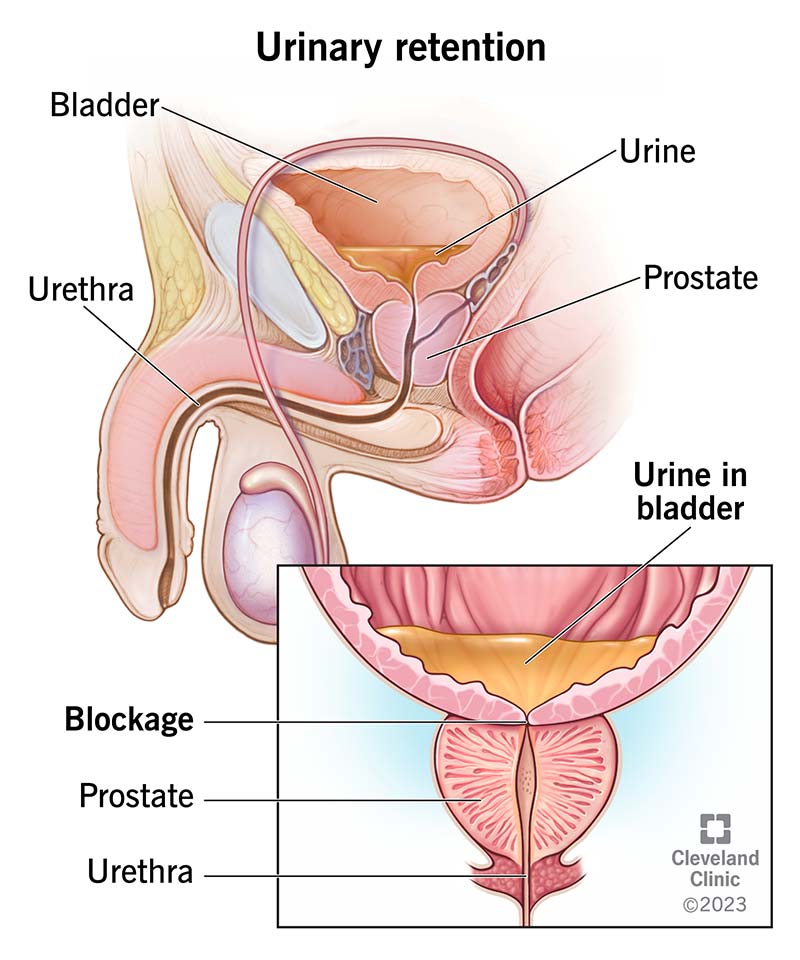
- Overflow Incontinence: Frequent or constant dribbling of urine due to a bladder that doesn’t empty completely. This can happen if there’s an obstruction (like an enlarged prostate) or if the bladder muscle is weak and can’t contract properly.
- Mixed Incontinence: A combination of stress and urge incontinence.
- Functional Incontinence: Physical or mental impairments prevent a person from reaching the toilet in time (e.g., severe arthritis, dementia).
- Transient Incontinence: Temporary leakage caused by a temporary situation like an infection, medication, or constipation.
Urinary Tract Diseases Linked to Uncontrolled Urination
Many underlying conditions affecting the urinary tract can directly cause or contribute to uncontrolled urination. Here are some of the most common ones:
- Urinary Tract Infections (UTIs): A common culprit, UTIs can irritate the bladder and urethra, leading to sudden urges to urinate, frequency, and sometimes incontinence. This is often transient and resolves once the infection is treated with antibiotics. Explore more about UTIs (Hypothetical link to NIDDK or similar trusted health site).
- Overactive Bladder (OAB): This is a specific type of urge incontinence where the bladder muscles contract too frequently and involuntarily, causing a sudden, strong urge to urinate that’s difficult to defer. While a symptom, OAB itself can be considered a chronic condition of bladder dysfunction.
- Enlarged Prostate (Benign Prostatic Hyperplasia – BPH): In men, an enlarged prostate gland can press on the urethra, obstructing urine flow. This can lead to overflow incontinence (bladder doesn’t empty fully, causing dribbling) or urge incontinence as the bladder tries to push past the obstruction.
- Weakened Pelvic Floor Muscles: Childbirth, aging, and obesity can weaken the pelvic floor muscles that support the bladder and urethra. This is a primary cause of stress incontinence, as these muscles are no longer strong enough to prevent urine leakage during physical exertion.
- Nerve Damage (Neurogenic Bladder): Conditions that damage the nerves controlling bladder function can lead to uncontrolled urination. These include:
- Multiple Sclerosis (MS)
- Parkinson’s Disease
- Stroke
- Spinal Cord Injury
- Diabetes (long-standing, poorly controlled)
- These conditions can disrupt the signals between the brain and bladder, leading to either an overactive bladder (urge incontinence) or an underactive bladder that doesn’t empty (overflow incontinence).
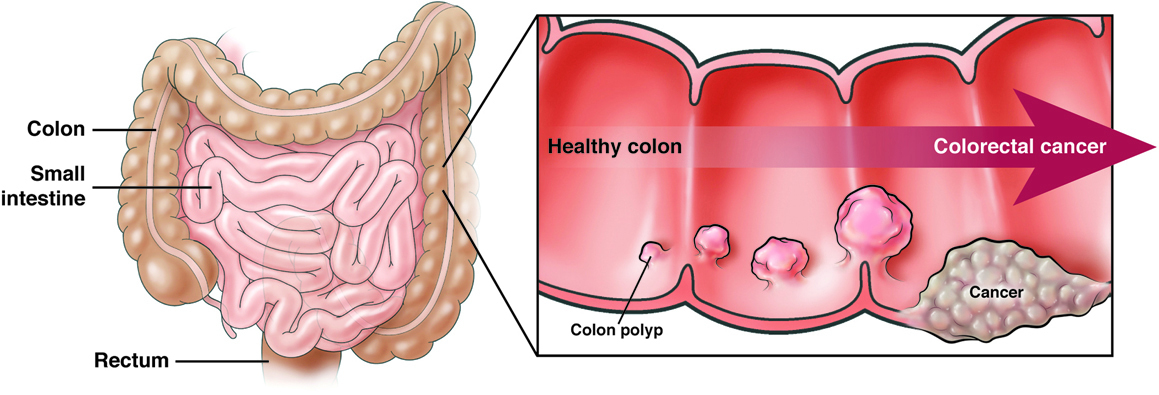
- Bladder Stones or Tumors: Less common, but stones or growths within the bladder can irritate the bladder lining, causing urgency and leakage, or even obstruction leading to overflow incontinence.
- Interstitial Cystitis (Painful Bladder Syndrome): This chronic condition causes bladder pain, pressure, and sometimes urgency and frequency, which can mimic or lead to symptoms of urge incontinence.
- Urethral Stricture: Narrowing of the urethra due to scarring from injury, infection, or inflammation can obstruct urine flow and lead to overflow incontinence.
Diagnosis and Treatment of Uncontrolled Urination
Given the varied causes, diagnosing the root of uncontrolled urination involves a comprehensive approach:
- Medical History and Physical Exam: Your doctor will ask about your symptoms, medical conditions, medications, and perform a physical exam, including a pelvic exam for women and a rectal exam for men (to check prostate).
- Urine Tests: Urinalysis can detect UTIs, blood, or other abnormalities. A urine culture can identify specific bacteria in case of infection.
- Bladder Diary: You might be asked to record fluid intake, urination frequency, and leakage episodes.
- Urodynamic Studies: A series of tests that measure bladder pressure and flow rates during filling and emptying.
- Cystoscopy: A procedure using a thin scope to look inside the bladder and urethra.
- Imaging: Ultrasound or MRI may be used to examine the bladder, kidneys, and surrounding structures.
Treatment for uncontrolled urination is highly individualized and depends on the specific cause:
- Lifestyle Changes: Fluid management, dietary modifications (reducing caffeine, alcohol), weight loss, and timed voiding schedules.
- Pelvic Floor Muscle Training (Kegel Exercises): Strengthening these muscles is crucial for stress incontinence and can help with urge incontinence. Find reliable Kegel exercise guides (Hypothetical link).
- Medications:
- For urge incontinence/OAB: Anticholinergics or beta-3 agonists can relax the bladder muscle.
- For overflow incontinence: Medications to shrink the prostate (for BPH) or improve bladder emptying.
- Medical Devices: Pessaries (for women) or urethral inserts can help manage stress incontinence.
- Minimally Invasive Procedures/Surgery: For severe cases of stress incontinence, surgical options like sling procedures can provide support to the urethra. For overflow due to obstruction, surgery to remove the obstruction might be necessary.
- Nerve Stimulation: For overactive bladder, sacral neuromodulation or posterior tibial nerve stimulation can help regulate bladder function.
Living with and Preventing Uncontrolled Urination
While uncontrolled urination can be a challenging condition, it’s highly treatable. It’s important to remember that it’s not an inevitable part of aging and should never be ignored due to embarrassment. Early diagnosis of the underlying urinary tract disease or condition is key to effective treatment and preventing potential complications.
Maintaining a healthy weight, avoiding bladder irritants, staying hydrated, and doing regular pelvic floor exercises can all contribute to prevention and better bladder health. If you experience any form of uncontrolled urination, speaking openly with a healthcare provider is the first and most important step towards regaining control and improving your quality of life.