Genital warts, HPV vaccine – this crucial question often arises for individuals diagnosed with Human Papillomavirus (HPV)-related conditions. Genital warts, caused by certain types of HPV, can be distressing, leading to concerns about future health and prevention strategies. While the HPV vaccine is widely known as a highly effective preventive measure, its role when someone has already contracted the virus or developed warts is a common point of confusion. This article aims to clarify the expert advice surrounding genital warts, HPV vaccine to empower you with accurate information.
Understanding Genital Warts and the HPV Virus
Before we delve into whether you can get the HPV vaccine with genital warts, it’s essential to understand what both entail:
- What is HPV? Human Papillomavirus (HPV) is a common virus with over 200 different types. Some types cause common warts, while others are sexually transmitted and can lead to serious health issues.
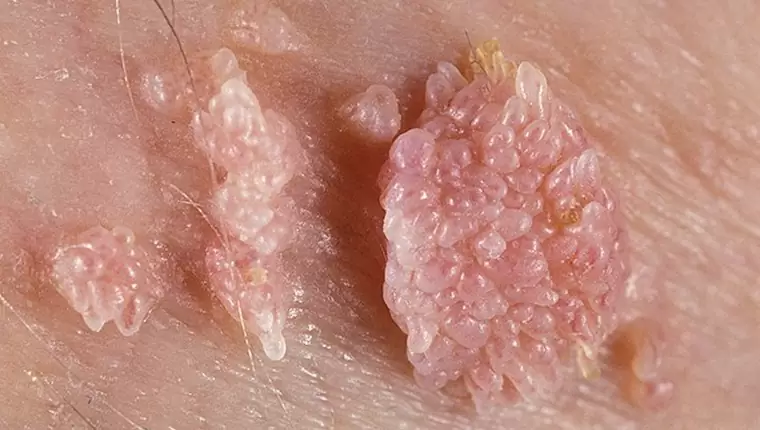
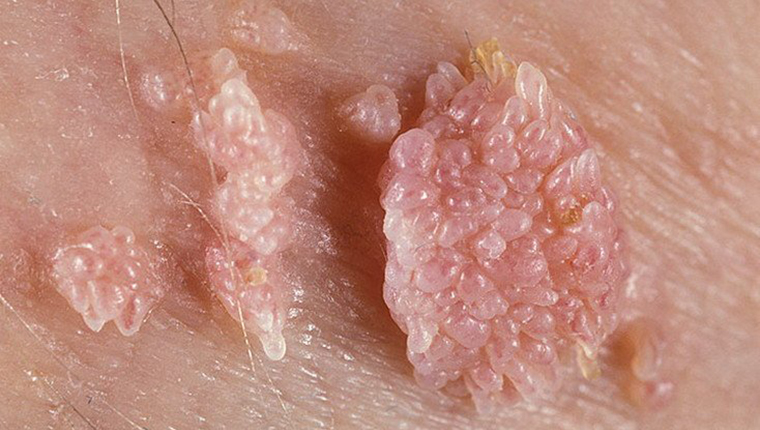
- Genital Warts: These are typically caused by low-risk HPV types, primarily types 6 and 11. They manifest as soft, fleshy growths that can resemble cauliflower or small bumps, commonly appearing on the genitals, anus, and sometimes in the mouth or throat. While generally not cancerous, genital warts can be persistent, uncomfortable, and emotionally distressing.
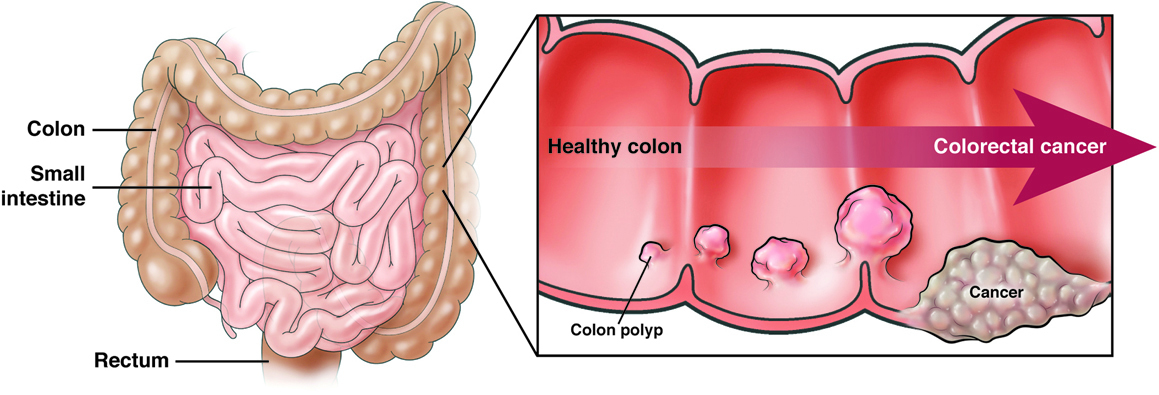
- High-Risk HPV Types (Cancer-Causing): Beyond the types that cause warts, about 14 HPV types are considered high-risk, with types 16 and 18 being the leading causes of cervical cancer, anal cancer, oropharyngeal cancer, and penile cancer.
Crucially, being infected with one HPV type does not grant immunity to others. It’s possible to be co-infected with multiple HPV types simultaneously. This fact is key when considering vaccination.
Can You Get the HPV Vaccine with Genital Warts? Expert Advice Says Yes!
The short answer to whether you can get the HPV vaccine with genital warts is: YES, YOU CAN AND SHOULD! Even if you have been diagnosed with genital warts, receiving the HPV vaccine offers significant benefits and is recommended by major health organizations worldwide. Here’s why:
- Protection Against Other HPV Types: Current HPV vaccines (like Gardasil 9) protect against nine of the most common HPV types. This includes the types that cause most genital warts (6, 11) and the high-risk, cancer-causing types (16, 18, 31, 33, 45, 52, 58). If you have only been infected with one or a few HPV types (typically 6 or 11, which cause warts), the vaccine will still protect you from the other types you haven’t been exposed to – especially the dangerous cancer-causing types. This is the most compelling reason for considering the HPV vaccine with genital warts.
- Reduced Risk of Re-infection/New Infection: Even if you have been infected with types 6 or 11, vaccination may help reduce the risk of re-infection with the same types if your body has cleared the virus, or lower the chance of new infection if you are re-exposed to the virus.
- Potentially Enhanced Immunity: Some studies suggest that the vaccine can produce a more robust immune response compared to natural immunity acquired after an HPV infection. This could potentially help your body fight off future exposures more effectively. However, it’s vital to remember that the vaccine is a preventive measure, not a treatment for existing warts or HPV-related diseases.
Important Note: The HPV vaccine does not treat existing genital warts or any other HPV-related conditions you may already have. Its primary purpose is to prevent initial HPV infection. Therefore, if you currently have genital warts, you will still need to undergo appropriate treatment for the warts as advised by your healthcare provider.
Who Should Get the HPV Vaccine and When?
The HPV vaccine is recommended for both males and females to protect against HPV-related diseases.
- Recommended Age Range:
- 9-14 years old: This is the ideal age for vaccination as the immune system responds best, and most individuals in this age group have not yet been exposed to HPV.
- 15-26 years old: Vaccination is still highly effective in this age group.
- 27-45 years old: Some national guidelines and medical recommendations permit vaccination in this older age group, particularly if the individual has not been vaccinated previously or is at high risk of exposure. Vaccination in this age range should be discussed with a healthcare provider to assess specific benefits and risks.
- Timing When You Have Genital Warts: You can get the vaccine even while you are undergoing treatment for genital warts or after they have been treated. It’s crucial to consult with your doctor for personalized advice on the appropriate vaccination schedule for your specific health situation.
Expert Recommendations When Dealing with Genital Warts
If you currently have genital warts, it’s vital not to panic but to seek professional medical advice and treatment from a specialist (dermatologist, gynecologist, urologist).
- Treat Existing Warts: Your doctor will recommend the most suitable treatment method for your existing genital warts (e.g., laser removal, cryotherapy, topical medications, surgical excision).
- Screening and Testing: You may be advised to undergo tests to determine the specific HPV types you are infected with and to screen for any pre-cancerous lesions (for women, regular gynecological exams and Pap smears are crucial).
- HPV Vaccine Consultation: Discuss with your doctor about getting the HPV vaccine to protect against other HPV types and reduce the risk of future infections.
- Practice Safe Sex: Always use condoms correctly and consistently to reduce the risk of transmitting or re-infecting with HPV, as well as other sexually transmitted infections.
- Inform Your Partners: It’s important to inform your current and past sexual partners (if possible) about your condition so they can get tested and seek treatment promptly.
In conclusion, the question of whether you can get the HPV vaccine with genital warts is clear: Yes, you can, and it is a beneficial measure for long-term health protection against other dangerous HPV types, especially those that cause cancer. Always be proactive in prevention and seek timely treatment to protect your own health and that of your community.